What if paralyzed limbs could move using only the power of one’s thoughts? Borrowing a story line from the realm of science fiction, a team of researchers at The Miami Project to Cure Paralysis — together with neurosurgeons and biomedical engineers from the University of Miami Miller School of Medicine — are using a brain-machine interface to make this once seemingly impossible feat a reality for people who are living with spinal cord injury (SCI).
Seeking innovative ways to restore function after SCI is one of the central goals of The Miami Project, which was founded in 1985 and has grown to become one of the “crown jewels” of the Miller School and a model for other institutions developing centers for SCI research.
On November 30, 2018, neurosurgeon Dr. Jonathan R. Jagid, associate professor of neurological surgery, and Abhishek Prasad, assistant professor of biomedical engineering, led a surgical procedure as part of an ongoing FDA-approved clinical trial in which an investigational system was implanted on the brain of a research participant.
The 22-year-old man, who sustained a SCI to his C5 vertebrae as a result of a motor vehicle accident several years earlier, is a complete quadriplegic — meaning he has no movement or sensation below the biceps and elbow — and in need of around-the-clock nursing care for many aspects of daily living.
Because the spinal cord carries information from the brain to the muscles that control the body, people with SCIs in their high cervical area are often left with the inability to use their hands or limbs. Remarkably, however — despite the fact that their brain signals no longer reach their target muscles — the cells in the brain still respond when a person even thinks about moving their hand.
For SCI researchers, though, the challenge has been trying to read those signals from the brain and bypass the injured spinal cord to achieve movement of a patient’s arms or legs. In the 1970s, Jacques Vidal, Ph.D., professor emeritus of computer science at UCLA, coined the term “brain-computer interface” as he began exploring ways brainwaves could be used to control external devices.
Research into human-machine interaction has exploded over the past few decades, as scientists from around the world look at ways to use non-invasive and permanently implanted sensors to record brain activity and control everything from screen cursors to robotic arms.
In a pre-clinical study published in 2018, Prasad and his team compared the feasibility of decoding movement information from the scalp of healthy control subjects and comparing that to patients who had a cervical SCI. They found that despite the damage to the spinal cord, the brain signals of both healthy subjects and SCI participants as recorded from the surface of the scalp contained sufficient information to determine with high accuracy when they wanted to initiate movement. Now, with sensors sitting on the surface of the brain, the decreased noise on the recorded brain signals is already leading to improved decoding results.
At the Miller School of Medicine, Jagid worked with neurosurgeon Dr. Michael Ivan, an expert in brain mapping, to stimulate different areas of the brain to identify the precise area that controls the research participant’s dominant right hand. Jagid and his team then implanted the device on that particular part of his brain.
“What’s unique here is that nobody to date has used this particular fully implanted device in an attempt to have an SCI patient achieve restoration of function that can potentially be used in a meaningful way outside of the lab,” Jagid said. “Other devices that have achieved similar results require a person to have an implanted post protruding from the head and tethered to a computer in a lab.”
“There’s no need for the patient to be hooked up to wires or connected to a device,” Ivan said. “It’s completely driven by their own thought process to stimulate this machine which helps in their daily activities of living.”
Following the surgery, the team spent weeks using a sophisticated program to “train” the computer to understand when thoughts of hand movement were observed in the electrical activity from the research participant’s brain. Within milliseconds of a signal being detected, special algorithms written by Noeline Prins, a postdoctoral research associate in the Department of Biomedical Engineering, and Dr. Iahn Cajigas, a resident in the Department of Neurological Surgery, determine whether he is thinking about moving his hand. Electrical signals are then sent to an external orthosis that stimulates the research participant’s hand muscles and causes them to open or close, much the same way that his body did before injury.
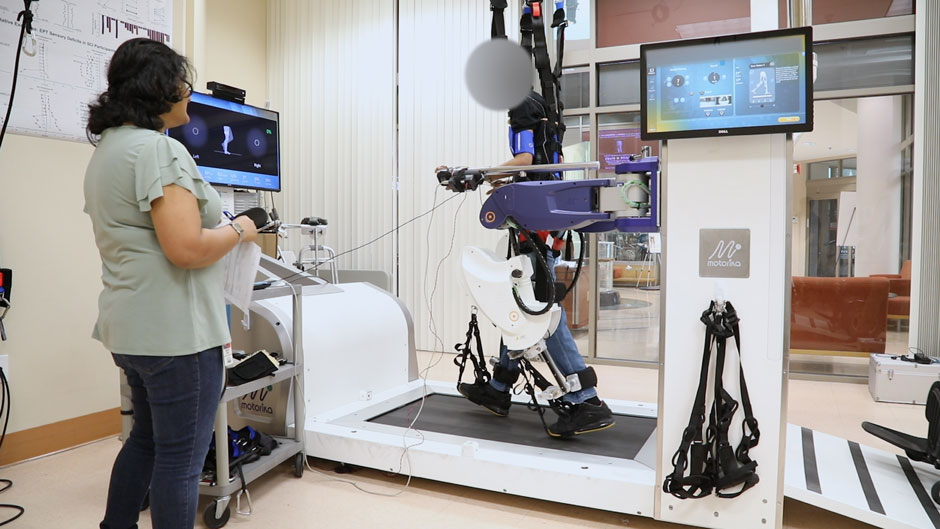
With this brain-machine interface, the research participant is able to successfully grasp and pick up objects with his right hand and move them from one place to another, and also write letters and words. Even more impressive, he has progressed to the point that he is now able to “walk” with the use of a robotic ambulator.
“The subject has had this device now for about three and a half months,” Jagid said. “We’re just amazed at how quickly he’s adapted to this technology, how easily he’s able to do things that he was unable to do before. We’re really ecstatic about the early results.”
Jagid and his team hope that, in the not too distant future as technologies such as this evolve, the effect of a devastating SCI can be minimized, giving patients the ability to live more independently.
“I think with this fully implanted device, with no external parts tethered to large computers in a lab, we are one step closer to restoring useful function to those suffering with spinal cord injury in a home environment improving quality of life,” Jagid said.
“As technology evolves, and devices get smaller, and computational power increases, the kind of things that we’ll be able to do to restore function is sort of limitless,” said Cajigas. “It really is up to our imagination as engineers to take what we understand of the neuroscience and connect the dots to get them to patients.”
Joining Jagid, Ivan, Prasad, Prins, and Cajigas for this clinical trial are Sebastian Gallo and Jasim Ahmad, undergraduate researchers, Department of Biomedical Engineering; Letitia Fisher, research coordinator; Anne Palermo, physical therapist; Audrey Wilson, research associate, and Steven Vanni, associate professor of neurological surgery.