Amid a global pandemic and with the flu season approaching, the ability to differentiate between various symptoms and proper care can be challenging. During a virtual conversation hosted by the University’s Division of Continuing and International Education, medical experts from UHealth and the American Heart Association weighed in on the differences between the diagnoses and shared advice on treatment.
Drs. Fredric W. Pullen, II, and Bjorn S. Herman, otolaryngologists for UHealth, and Dr. Marcos Sanchez-Gonzalez, an expert in cardiovascular physiology and director of continuing medical education at Larkin Community Hospital, led the discussion and offered insight into the impact of allergies. All three doctors instruct the Division’s Allergy Diagnostics and Allergen Immunotherapy Training Workshop.
“Part of the problem with allergies is that there are more than 50 million Americans with allergic diseases,” said Dr. Pullen. “It is the sixth leading cause of chronic disease in the United States, and it is the leading cause for children.”
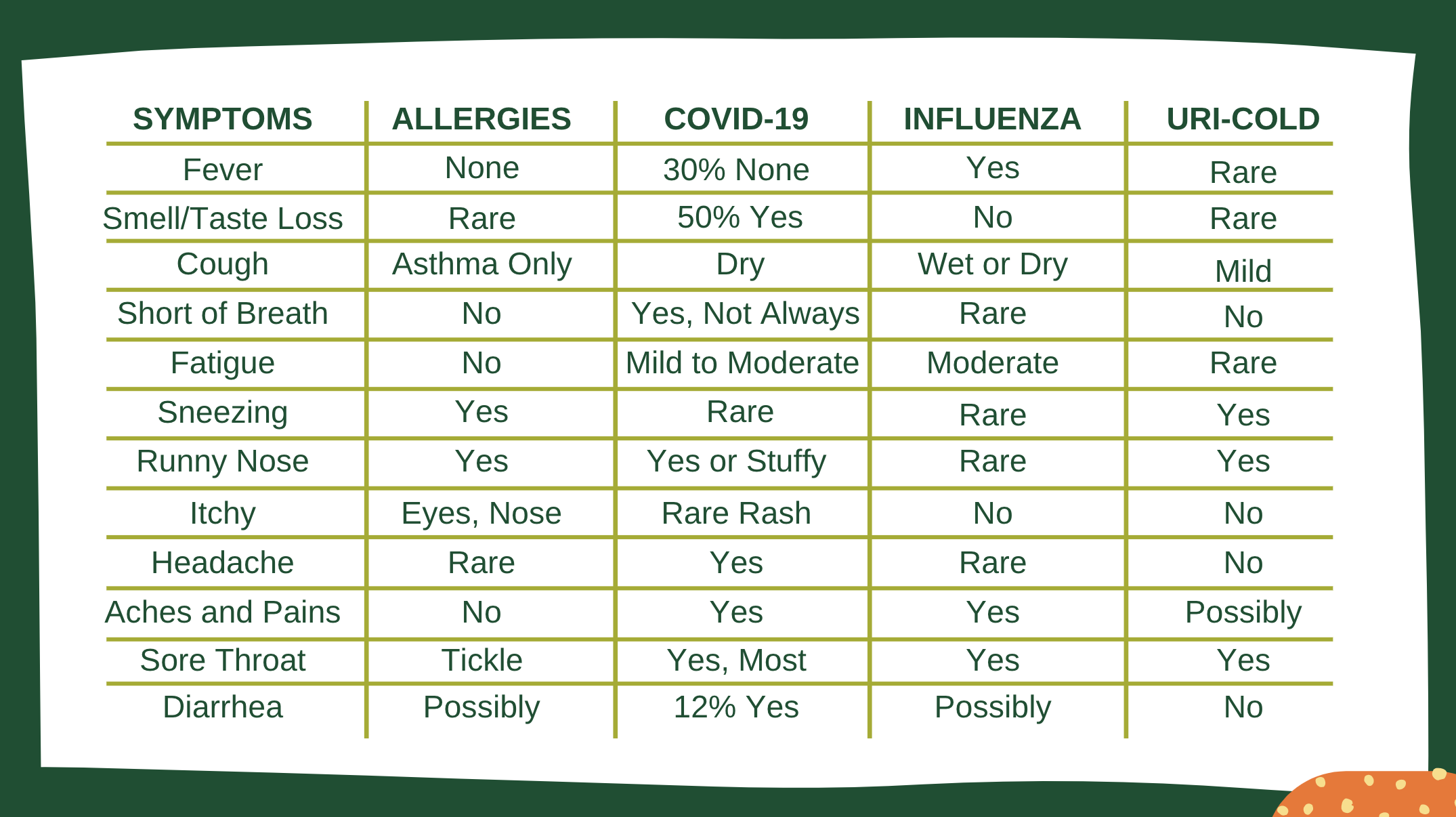
In addition, allergies often contribute or co-present factors in conditions treated by other specialists, including pulmonologists and otolaryngologists, dealing with COVID-19, according to Dr. Pullen. During the virtual event, he outlined the symptomatology observed in allergies, COVID-19, influenza, and upper respiratory infections (URIs). He noted that some of the most critical differentiators are whether a fever, dry cough, or loss of taste and smell is present in the patient. While the loss of taste and smell does not occur in influenza and is a rare occurrence in allergies and URIs, 50 percent of those with COVID-19 do, indeed, experience that loss.
To emphasize how the similarities between the symptoms of COVID-19 and allergies make it difficult to tell the difference between them, Dr. Herman presented two case studies. The first was a woman, 61, with a history of seasonal allergies who experienced no fever or shortness of breath but several days of nasal congestion, runny nose, and a mild, intermittent cough that she attributed to post-nasal drip. The second was a woman, 40, who experienced a loss of smell and decreased taste over several days but no fever, cough, shortness of breath, nasal congestion, or headache.
“I think most people who know that the loss of smell and taste is an issue would probably say the second person tested positive for COVID-19, but in fact, both of these patients tested positive for COVID-19,” said Dr. Herman. “The key here is that the first person’s husband had COVID-19. It is essential to screen and ask about history because something that seems very straightforward, like allergies, can manifest as another disorder, including COVID-19.”
In addition to allergies, the upcoming flu season also presents challenges. While the flu and COVID-19 share many similarities, health experts—including Dr. Julio Frenk, the University’s president—strongly encourage everyone to get the flu vaccine to help lessen the confusion of symptoms and the possibility of the two viruses interacting. All faculty, staff, and students at the University are required to receive a flu shot.
Read: Flu vaccinations mandatory for the University community
In terms of the adverse health effects of untreated or poorly controlled allergies, Dr. Sanchez-Gonzalez shared that there has been an increase in cases of patients who have experienced complications because of a lack of treatment for their allergic disorders. Since the pandemic forced many clinics to close during the quarantine, fewer patients have had access to allergy treatment, including allergy immunotherapy shots. Consequently, patients with these poorly managed chronic conditions have been experiencing complications and inundating emergency rooms.
Robert Hill Jr., vice president of health strategies for the American Heart Association, shared that 23 percent of people hospitalized for COVID-19 had experienced serious cardiovascular complications. He noted that while the pandemic has disrupted the ability to receive allergy treatment, it has also disrupted general routines that include exercise activities, leading to a domino effect that contributes to high blood pressure and increasing obesity.
“There is a link between allergies and cardiovascular disease,” said Dr. Sanchez-Gonzalez. “The higher the level of allergies, the more prevalent cardiovascular disease becomes. The simple way to understand this relationship is by understanding the role of inflammation. Uncontrolled inflammation is the common denominator. One allergic event may not be enough to cause severe complications. But sustained, chronic allergic inflammation can end up affecting the cardiovascular system and impair quality of life.”
As allergies continue to be unavoidable for many, University and CDC guidelines are currently in place to lessen the spread of COVID-19 and protect the community from the seasonal flu. Learn more about how to schedule your flu shot by visiting coronavirus.miami.edu/flushot.
About the University of Miami Division of Continuing and International Education
The Division of Continuing and International Education at the University of Miami aims to empower people to reach their full potential through lifelong and lifewide learning. With more than 70 credit and non-credit programs available, the Division focuses on creating continuous learning experiences that transform individuals, organizations, and entire communities. For more information, visit dcie.miami.edu and connect with the Division on Facebook and Twitter. To speak with an enrollment advisor about the Division’s Allergy Diagnostics and Allergen Immunotherapy Training Workshop endorsed by the Academy of Allergy & Asthma in Primary Care, call 305-284-4000.

